RevKeep Software automates healthcare payment audits and EHR data extraction, helping providers and all partners save time, prevent losses, and work smarter .
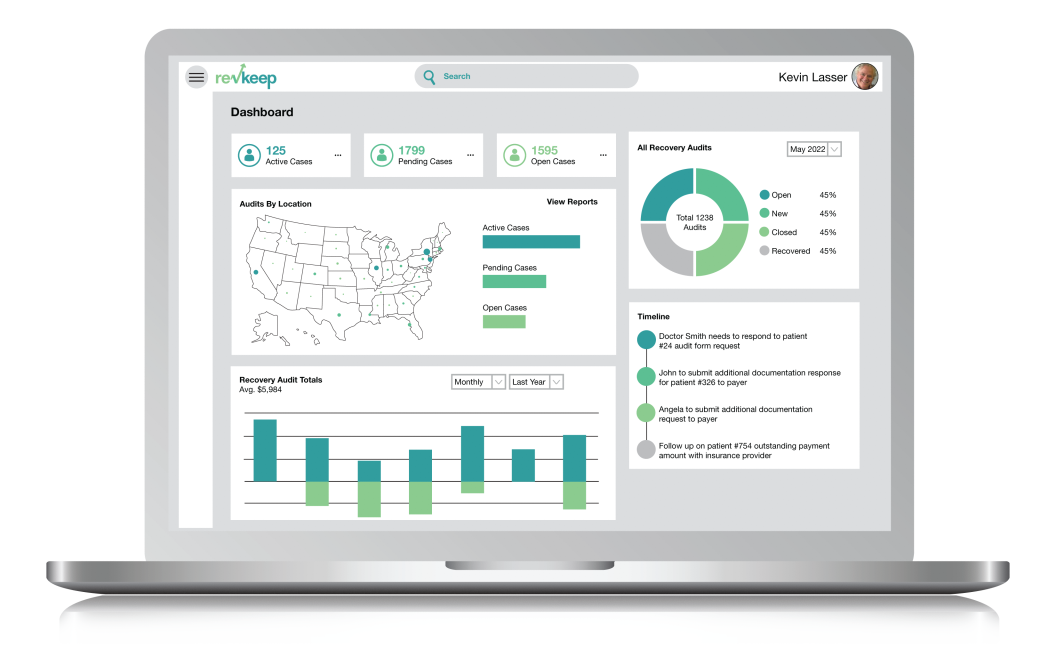
Our RAC and private payor audit solution helps your revenue cycle management team stay ahead of requests. With our push notifications if someone is on vacation, responding to audits is no longer person-centric. Access patient records instantly, respond quickly, and retain more of your hard-earned revenue.

Work seamlessly with hospital EHRs to gather critical records, strengthen cases, and deliver results to keep previously earned money. No more slowdowns, no more missing data.
In a world of shrinking teams and growing audit demands, it’s easy to fall behind. Miss a deadline, and you lose the money—simple as that. RevKeep transforms this struggle into a streamlined, efficient process.
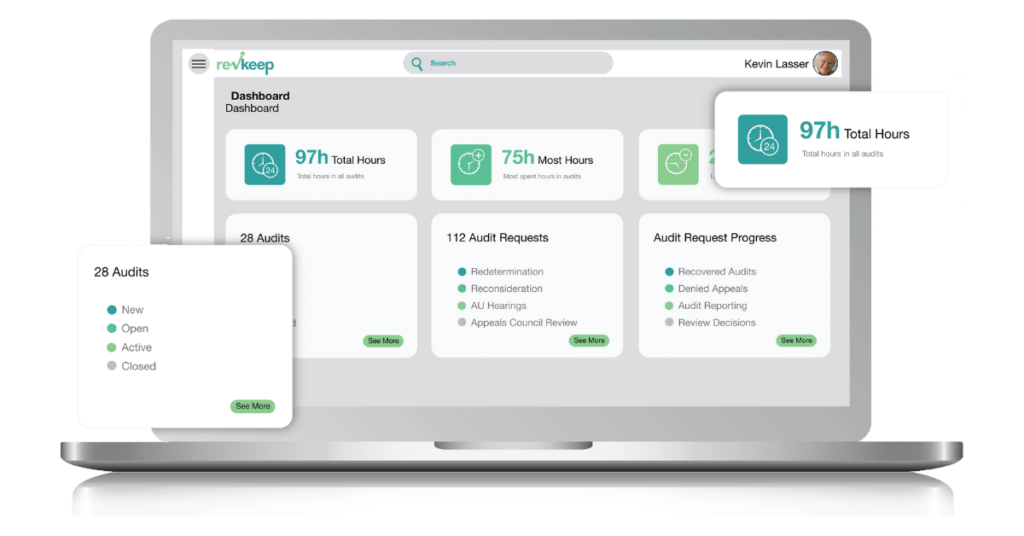
No more digging through spreadsheets or juggling multiple platforms. With RevKeep’s customizable dashboards, you get immediate visibility into every audit and data request. Create charts, track trends, and filter by team member or department. Easily collaborate—remote or in-office—to ensure everyone stays aligned, informed, and ready to act.
Our clients see real results:
In a world of shrinking teams and growing audit demands, it’s easy to fall behind. Miss a deadline, and you lose the money—simple as that. RevKeep transforms this struggle into a streamlined, efficient process.
We’re responsive, nimble, and truly care about your success. Our solution isn’t just software—it’s personalized support, from onboarding to ongoing optimization.


Don’t let complexity hold you back. Automate, secure, and streamline your audit and legal processes starting today.